Until vaccines become much more widely available, prevention and harm reduction are important strategies
As more than 75 countries have confirmed over 25,000 Monkeypox cases in non-endemic countries, a myopic hysteria has seized public health experts, the LGBTQIA+ community, and conservatives attempting to weaponize the moment.
At the root of this hysteria seems to be racist and homophobic biases, a lack of Western understanding about the history of Monkeypox, county-specific underreporting issues, testing bottlenecks, vaccine stockpiling red tapes, treatment impediments, and crisis fatigue.
As we collectively continue to follow this outbreak, here is information relevant to understanding, preventing, treating, and educating yourself and others about this outbreak.
Quick History and Facts:
First identified in 1958, Monkeypox (MPX), which many health care professionals stress needs to have a name change to avoid stigma, is currently considered endemic in ten African countries. It has been around for six decades and has never been considered an STD, Jackson Memorial Hospital medical director, Dr. John Esin, stressed.
The self-contained virus tends to last two to four weeks with fatality rates around three to six percent. The incubation period (from infection to beginning of symptoms) is six to thirteen days.
For this outbreak, the virus doesn’t look like it does in textbooks. Often, it can take the form of one or two lesions easily confused for STIs such as herpes or syphilis. Textbook symptoms describe a flu-like illness with fever, fatigue, and swollen lymph nodes. A rash soon follows with painful blisters that spread across the body.
The rash seems to centralize in the genitals or anus and doesn’t always spread. For some, instead of a pox, there are ulcers or craters. Still, the pain can require medication and the sores may cause long-term scaring.
Until recently, it was rare in Europe and the Americas, according, to Smithsonian Magazine. Arguably, MPX in Africa is the result of unequal access to global vaccine stockpiles and other healthcare resources, discussed below.
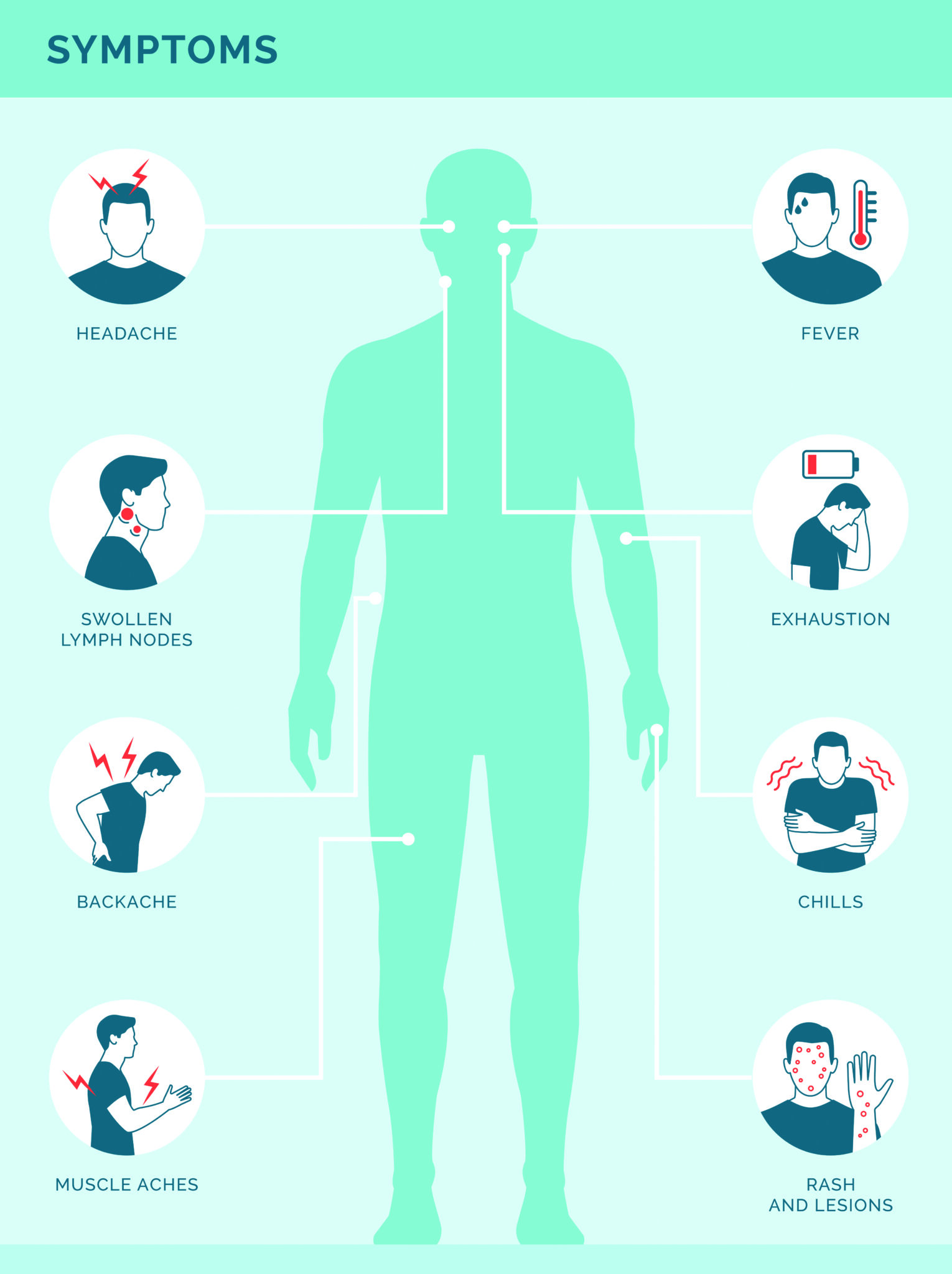
Spread:
The virus spreads through direct contact with an infected person’s bodily fluids, sores, or scabs and sharing contaminated objects, such as clothing or bedding. While airborne exposure is possible but less common and understudied.
Currently, the virus seems to be spreading mainly among men who have sex with other men (MSM). Importantly, smaller number of pediatric cases have been reported.
Science Magazine suggests this spread among MSMs could be due to a “highly interconnected sexual networks.” In fact, epidemiologist Mateo Prochazka, who consults for the United Kingdom Health Security Agency, emphasized that transmission risk is “less about sexual identity and more about sexual networks.”
The ability to respond to these trends has been further hobbled by a combination of long-neglected historical facts and deeply rooted scrutiny of sexual minorities.
Vaccine Stockpile Concerns:
Citing a 2004 letter by then Secretary of Health and Human Services, Tommy G. Thompson, where the United States pledged 20 million smallpox vaccines to the global stockpile managed by the WHO, the consumer advocacy non-profit, Public Citizen, urged the United States to expedite releasing the 100 million smallpox vaccines in its global stockpile, “an older generation of smallpox vaccine believed to be [85 percent] effective against monkeypox,” according to the Washington Post.
Despite the massive smallpox vaccine stockpile, the federal government has been hesitant to distribute vaccines to states and counties. The CDC also recommends that people with weakened immune systems or certain skin conditions should not take it unless exposed.
Conversely, Jynneos was approved for prevention of smallpox and monkeypox in 2019. The company that developed Jynneos, Bavarian Nordic, indicated that the United States government exercised a $119 million order, according to the Washington Post.
The biotech company also indicated several new lucrative deals with undisclosed countries, prompting two upgrades to its financial guidance, as indicated by Reuters.
Prevention
Until vaccines become much more widely available, prevention and harm reduction are important strategies against the illness.
Talk to your partner(s) about recent illnesses and be vigilant of unexplained rashes, especially the genitals and anus. If there any recent flu-like illnesses or rashes, avoid sex and contact a healthcare provider, including public health clinics near you.
Individuals are encouraged to call providers, not walk in in-person. Screening for STIs is also important because California health experts indicated a 25 percent concomitant infection rate between Syphilis and Monkeypox infections.
The best protections are to avoid any form of sex (oral, anal, vaginal); do not kiss or touch each other’s bodies while sick, especially avoiding any rashes. Do not share towels, fetish gear, toys, or toothbrushes.
Harm reduction strategies include considering virtual sex options with no in-person contact. Cover areas where rash is present, reducing as much skin-to-skin contact as possible. Condoms may help prevent the spread of rashes confined to genitals but aren’t likely enough coverage to prevent Monkeypox. Remember to wash any shared items after use. Avoid or limit new, multiple, or anonymous sex partners. Lastly, if you think you are infected, avoid touching your rash, otherwise it may spread to other parts of the body and delay healing.
Vaccination
Currently, California has received more than 61,000 doses, of which the state has distributed over 25,000, according to a press release from Governor Gavin Newsom declaring a state of emergency to combat Monkeypox. Tracking California’s response can also be reviewed online, at the California Department of Public Health.
Two vaccines are currently available. Jynneos was previously approved by the FDA and ACAM2000 is approved under the Expanded Access Investigational New Drug application, but should not be used in people with weakened immune systems, skin conditions, or who are pregnant, according to the CDC.
Vaccines are slowly made available to states, who then distribute them to local health care agencies and counties. Some counties, such as Los Angeles, already had a working relationship with the national stockpile so they get their supplies directly.
Jynneos doses are administered over two doses, intended to be one-month apart. The maximal immune response development takes 14 days after the second Jynneos dose and four weeks after the ACME2000 dose. Though many health agencies have indicated prioritizing first dose shots.
According to the CDC, vaccine side effects are generally mild, more likely to occur in people with chronic skin conditions and those who are immune compromised. Side effects may include:
- Soreness or redness at injection point.
- Armpit glands may swell and be sore.
- Slight fever.
- One out of three people feel sick enough to call out of work.
- One in a thousand may experience more severe effects.
Treatment:
At a California Department of Public Health zoom update this week, health experts stressed that treatment, Tecovirimat (TPOXX), options were available, but currently hampered by burdensome paperwork, which they hoped a declaration of emergency may relieve.
Unlike vaccine options, which are currently restricted to those 18 years of age and older, treatment is available to those under 18, but state officials emphasized it was not a “straightforward process”.
San Diego
Patrick Loose, head of the San Diego County HIV, Hepatitis, and HIV branch, indicated the County had received 3,987 vaccines and have distributed 2,415 as of August 1.
Of the vaccine appointments available, 200 were in the weekday evenings (5:30 pm to 8 pm). Currently contracted HIV outreach providers will be charged to include “monkeypox health & risk reduction education at the bathhouse twice per month,” according to Loose.
Many new vaccine shipments are “being distributed to health care systems and federally qualified health centers so those organizations can provide post-exposure prophylaxis for their patients.”
In discussing the county’s request for more vaccines, Loose indicated the county’s low verified case count, currently at 27 as of August 1, limited the state from allotting more vaccines.